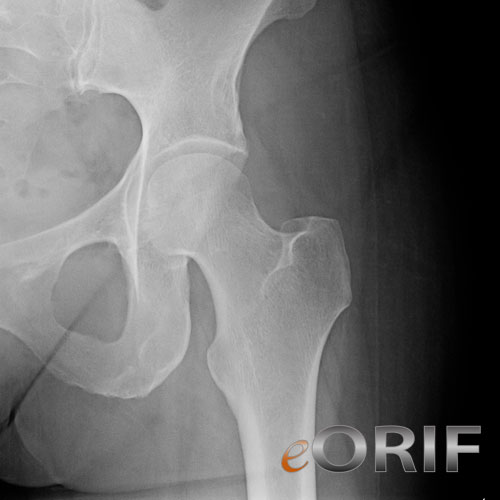
The following points should be kept in mind when performing radiographs of orthopedic fixation hardware. One only has to look at the outside films taken at the offices of most nonradiologists to see what kind of difference we make by monitoring such mundane matters as processor chemistry, cassette cleaning, film densitometry, etc. Therefore, it must be the radiologist who monitors the imaging workup and suggests the most efficacious and cost-effective followup imaging studies for each patient.Īnother important role of the radiologists is film quality control. They are likewise on much shakier ground when it comes to understanding the underlying physics, indications, and interpretation of radionuclide bone scans, fluoroscopy, ultrasound, CT and MRI. It is the radiologist’s job to look closely for these entities. Although orthopedists as a group do a superb job of interpreting plain radiographs on trauma patients, they tend to do much less well as a group when it comes to other disorders, such as metabolic bone disease, infection, neoplasms or arthritis. However, we do know imaging better than they do. So, how can radiologists add some value to the examination? We are never going to know the history, physical findings, surgical findings and postoperative course as well as the orthopedists do. I would hate for this to happen at UW, because the great majority of my practice consists of studies ordered by orthopedist. Health plan managers and third-party payers are increasingly under the gun to reduce health care costs, and it is hard to argue that radiologists should continue to receive compensation for zero-content dictations. In some hospitals, they have been successful. In a growing number of medical centers across the country, orthopedists are pressing their hospital administrations for the right to bill for film interpretation and to cut the radiologists out of the loop completely. This tendency for radiologists to tap dance their way through orthopedic dictations has not gone unnoticed by the orthopedists. If you are going to bill for the dictation, you should say something intelligent about the film and add some value to the examination. I think that this kind of dictation is a real disservice to the patient, especially if you are charging for it. Yellow: The acetabular roof can be easily visualized.For some reason, many radiologists freak out when they are faced with reading out films with orthopedic hardware, and will mumble something vague along the lines of “Orthopedic hardware is seen and surgical changes are noted….”, for fear that they will say something dumb and the orthopedists will laugh at them. Pink: The outline of the obturator foramen is completely visualized. The posterior border can be followed cranial to identify the supra-acetabular surface, the gluteus medius pilar and the landmarks associated with the external surface of the innominate bone. Green: The posterior border of the acetabulum is easily visible due to the rotation of the anterior rim away and thus out of line for super-imposition. Additionally, time should be spent identifying the anterior superior iliac spine, the anterior inferior spine, the psoas gutter, and the pubic spine. The periarticular region of the anterior column is seen clearly. The pelvic brim and the represented periarticular anterior columnĪdditionally, the iliac wing can be visualized in cross section and most of the landmarks associated with the internal and external surface identified.īlue: The pelvic brim is demonstrated in blue.There are four consistent landmarks that should be inspected on the obturator oblique in each case:
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
